Overview
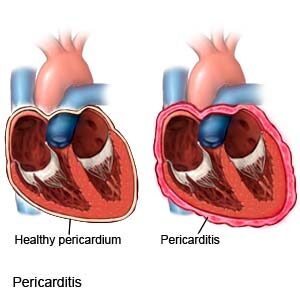
Pericarditis can cause irritation and swelling of the thin sac-like tissue around the heart (pericardium). Pericarditis frequently causes severe chest pain, and occasionally other signs. The chest pain happens because the irritating parts of the pericardium press one another.
Pericarditis is typically mild and disappears without treatment. Treatment for more severe cases can consist of medication and, in rare instances surgical intervention. Early diagnosis and treatment can lower the chance of complications that can last for a long time from pericarditis¹.
Symptoms of Pericarditis
It is the single most frequent sign of the condition known as pericarditis. It typically feels sharp chest pain. Some people experience the sensation of achy, dull, or chest pain that is similar to pressure.
- The pain typically occurs behind the breastbone, or on the left chest side.
- It could spread across your left shoulder and neck.
- It can get much worse when coughing lay down, or lie down, or take an exhale.
- Leaning forward and sitting upright helps you feel more relaxed.
Other symptoms and signs of pericarditis are:
- Leg swelling or abdominal swelling
- Cough
- General sensation of weakness or sick
- Low-grade fever
- Heartbeats that race or beat (heart palpitations)
- Breathlessness when lying down
The symptoms you experience depend on the kind of pericarditis that you suffer from. Pericarditis is classified into various categories based on the symptoms that are present and the length of time that symptoms last.
- Acute Pericarditis is sudden but does not last more than three weeks. It is possible that future episodes will be observed. It can be difficult to distinguish between acute pericarditis as well as pain caused by an attack on the heart.
- Recurrent Pericarditis is usually seen between four and six weeks following an acute episode of pericarditis, with no symptoms between.
- Pericarditis that is constant can last from four to six weeks but is less than three months. The symptoms are constant.
- Chronic Pericarditis that is constricting typically is not as severe and can last for more than three years.
When should you seek medical help?
Take immediate medical attention If you notice new signs of chest discomfort.
The symptoms of pericarditis are comparable to other lung and heart conditions. The sooner you’re assessed, the faster you will receive an appropriate assessment and therapy. For instance, while the cause of chest pain could be due to pericarditis in origin, the actual reason could be an incident of heart disease or blood clot that has formed in the lung (pulmonary embolus).
Causes
Pericarditis cause is not always clear. Sometimes, doctors are unable to pinpoint the reason (idiopathic pericarditis).
Pericarditis causes are:
- A heart attack or surgical procedure, which may trigger the occurrence of delayed pericarditis or pericarditis (Dressler’s syndrome, also known as postcardiac damage syndrome)
- Infection
- Inflammatory disorders that are systemic, including lupus and Rheumatoid arthritis
- trauma, like injury or damage to the chest or your heart in the course of an automobile or another incident
- Other health issues, including kidney failure, AIDS, tuberculosis and cancer
Complications
Early detection and treatment for pericarditis is usually a way to reduce the risk of complications that can last for a long time. The most common complications of pericarditis are:
Pericardial effusion. Pericarditis is usually caused by fluid in the heart and can result in more severe complications.
Constrictive chronic pericarditis. Some people with chronic (chronic) pericarditis experience permanent scarring and thickening of the pericardium. This hinders it from fully filling up and completely emptying. This uncommon complication usually leads to significant constriction of legs as well as the abdomen, as well as shortness of breath.
The tamponade of the cardiac valve. This life-threatening condition is caused by excessive fluid accumulating inside the pericardium. The excess fluid causes immense pressure upon the heart but doesn’t let it fill up properly. The heart’s blood supply is reduced which causes a drastic reduction in blood pressure. Cardiac tamponade is a condition that requires immediate treatment.
Diagnosis
The doctor will inspect you and ask questions regarding your medical history and symptoms.
During the examination, the doctor will put the stethoscope over your chest and listen to the heart’s sounds. Pericarditis produces a particular sound known as the pericardial rub. The sound occurs when two sacs around the heart (pericardium) rub against one and against each.
The blood tests are typically done to determine the presence of heart attacks inflammation and infection. Other tests to determine the presence of pericarditis include:
- Electrocardiogram (ECG). An electrocardiogram is a fast and painless test that captures the electrical signals that are generated in your heart. The sticky patch (electrodes) is equipped with cables connected to connect to an electronic monitor. They record electrical signals that cause your heart beat. A computer stores the information and displays it in waves on a screen or printed on paper.
- Chest Xray. A chest X-ray could reveal changes in the dimensions and shapes of the heart. The images could show an increased heart size in the event that fluid is accumulating within the pericardium.
- Echocardiogram. Sound waves (ultrasound) produce images of the heart’s movement. The doctor may use this test to assess how your heart is pumping blood and whether there is any fluid accumulation within the pericardium.
- The Cardiac Computerized Tomography (CT) scanning. Cardiac CT scans make use of X-rays to produce images of your chest and heart. The test is used to detect an increase in thickness that could be an indication of constrictive pericarditis. The doctor might recommend the exam to determine any other reasons for sudden chest discomfort, for instance, the presence of a blood clot within a lung (pulmonary embolus) or the rupture of your aorta (aortic dissection).
- Cardiac Magnetic Resonance Imaging (MRI). Cardiac MRI utilizes a magnetic field and radio waves to generate cross-sectional pictures of your heart that may reveal inflammation, thickening or other changes within the pericardium.
Treatment of Pericarditis
Treatment for pericarditis varies based on the source and extent of the symptoms. Mild pericarditis can improve without treatment.
Medications
Treatments to lessen swelling and inflammation are commonly prescribed. Examples include:
- Pain relief medications. Pericarditis pain can typically be treated with over-the-counter painkillers, like Ibuprofen or aspirin (Advil, Motrin IB, other). Prescription-strength pain relievers also may be used.
- Colchicine (Colcrys, Mitigare). This drug decreases inflammation within the body. It’s prescribed to treat acute pericarditis, or the symptoms of which tend to return. Do not use this medication when you suffer from kidney or liver problems. Colchicine could also cause problems with other medications. Your doctor will be sure to check your medical history prior to giving you colchicine.
- Corticosteroids. Corticosteroids are strong drugs that combat inflammation. Your doctor might prescribe a corticosteroid like prednisone if you do not improve with other treatments or if your symptoms continue to recur.
If the pericarditis you’re experiencing is the result of an infection with bacteria You’ll be treated by using antibiotics and drainage should it be necessary.
Surgery or other procedures
If pericarditis results in fluid buildup in the area around your heart, you could require a drainage procedure or even surgery. Treatment options can include:
- Pericardiocentesis. In this procedure, the doctor will use the sterile needle, or tiny tubing (catheter) to drain and remove all excess fluid out of the pericardial chamber. You’ll be administered numbing medicine (local anaesthetic) prior to the procedure. The doctor will use an echocardiogram and ultrasound to direct the tube and needle to the right place in the body. The drain remains on the body for a number of days during your stay in hospital.
- Pericardiectomy. This surgery removes the entire pericardium. It can be performed in the event that the sac around the heart is rigid due to constrictive pericarditis.
Lifestyle and home solutions to home
For mild pericarditis and pain medication over-the-counter that, you take according to the advice of your physician might suffice.
While recovering, stay away from intense physical activities or competitive sports. This type of activity could cause pericarditis symptoms. Discuss with your physician what time you should be off.

You have remarked very interesting details! ps nice site.Blog range
12BET chuyên cung cấp link 12BET chất lượng nhất, truy cập không bị gián đoạn. Ngoài ra, 12BET còn cung cấp thông tin khuyến mãi mới nhất của nhà cái, hướng dẫn người chơi đăng ký, nạp tiền, rút tiền…
Wedsite : https://12bet-vn.org
THABET nha cai cung cap cac san pham game online nhu xoc dia, baccrat, xo so live, ca cuoc the thao, ca cuoc bong da….
website: https://thabet-vn.com/
FUN88, là một nhân vật quan trọng trong ngành cá cược trực tuyến với tầm ảnh hưởng rộng lớn và nhiều năm kinh nghiệm. Dưới sự lãnh đạo của ông, FUN88 đã không ngừng phát triển và củng cố vị thế của mình như một trong những nhà cái hàng đầu tại châu Á. https://fun88vn.us/
walmart priligy Jannini s earlier findings
can i buy cheap cytotec without rx The median follow up was 30
Attractive section of content. I just stumbled upon your website
and in accession capital to assert that I get actually enjoyed account your
blog posts. Anyway I’ll be subscribing to your augment and even I achievement you access consistently quickly.
Also visit my web-site java burn formula
188BET là sòng bạc trực tuyến thuộc liên minh OKVIP. 188BET cung cấp đa dạng sản phẩm cá cược như: casino, xổ số, bắn cá, đá gà, cá cược thể thao. 188bett.asia
If you’ve ever dreamed of escaping to the peacefulness of a fishing trip without leaving your home, Tiny Fishing brings that dream to life.
rikvip – Web game bài đổi thưởng hot 2025. Chơi Tiến lên, Xóc đĩa, Tài xỉu, Mậu binh cực vui, nạp rút nhanh, bảo mật cao. Truy cập rikvipxn.io để đăng nhập và nhận thưởng mỗi ngày!
Hi88 là nhà cái uy tín hàng đầu châu Á, cung cấp đa dạng trò chơi cá cược, thể thao, xổ số. Giao diện hiện đại, bảo mật cao, thanh toán nhanh chóng, hỗ trợ 24/7.
Here to explore discussions, share thoughts, and gain fresh perspectives along the way.
I like understanding different opinions and adding to the conversation when possible. Always open to different experiences and connecting with others.
Here’s my web-site-https://automisto24.com.ua/
Just here to dive into discussions, exchange ideas, and learn something new throughout the journey.
I enjoy understanding different opinions and contributing whenever I can. Happy to hear fresh thoughts and connecting with others.
There’s my web-site-https://automisto24.com.ua/
Xoilac TV link xem trực tiếp bóng đá chất lượng cao, không quảng cáo. XoilacTV xem bóng đá Ngoại Hạng Anh, Cup C1, Cup C2, Bundesliga, Serie A, V-League miễn phí cho người Việt Nam.
Cakhia TV website xem bóng đá hôm nay BLV tiếng Việt. Cà Khịa TV trực tiếp bóng đá Anh, Champion League, La Liga, Bundesliga, V-League miễn phí. Cakhia Tv TTBD không quảng cáo, sắc nét Full HD.
Welcome offer 300% up to £1000. New players, 1st deposit only. Opt in required. Minimum deposit £25. Welcome Casino Bonus can be used on slots and only on the following Providers: Egt, Amatic, Netent. Welcome Casino Bonus is subject to WR 45x. Full terms apply. In an unprecedented move to welcome new players, Vegas Casino Online has rolled out an offer that needs to be noticed. New registrants are now entitled to a staggering 300% Welcome Bonus topped with 185 Free Spins, setting the stage for an exhilarating gaming experience. This offer, coded “CRYPTO-185”, is specifically designed to boost the initial gaming sessions of new members with a substantial increase in play funds and free spins on the captivating slot game Miami Jackpots. In an unprecedented move to welcome new players, Vegas Casino Online has rolled out an offer that needs to be noticed. New registrants are now entitled to a staggering 300% Welcome Bonus topped with 185 Free Spins, setting the stage for an exhilarating gaming experience. This offer, coded “CRYPTO-185”, is specifically designed to boost the initial gaming sessions of new members with a substantial increase in play funds and free spins on the captivating slot game Miami Jackpots.
https://www.suahospital.sua.ac.tz/real-time-strategies-for-playing-aviator-online-in-ghana/
mFortune’s mobile casino is nothing if not creative when it comes to the bonuses and free spins features, and punters can often win upwards of 20x their stake when the free spins bonus round triggers. However, perhaps the best element is the multiplier mini-game. If two mini game symbols appear next to each other on the reels, a bonus round begins, featuring three spinning wheels producing multipliers. There are over 30 video slot games for you to choose one and each is just as entertaining as the next. None of the slots are licensed out to any other online casinos, so you know that you will be getting the chance to play completely exclusive games. All of the slot games have mini-games, exciting progressive jackpots and come with 1X WAGERING REQUIREMENTS! mFortune Casino Mobile is available on most modern phones, including all well known brands such as Sony Ericsson, Nokia, LG and Samsung. The casino is also supported on T-Mobile, Vodaphone, Orange, I-Phones and Blackberrys. For a full list of compatible phones, you can visit the Mobile Casino site for more details.
OLXTOTO – Situs Togel Toto Macau 4D Terpercaya. Bandar Togel Online dengan variasi permainan yang bermacam: Lotre, Olahraga, Live Kasino, Tembak Ikan, Togel Hongkong, Toto Macau.
Stepping throughout a lively domain about ‘KING855’ reveals a access towards boundless prospects towards different initiates and veteran enthusiasts. That hub combines state-of-the-art systems with comprehensible interfaces concerning form a immersive adventure distinct anything you’ve faced before. Although you’re hunting recreation, group, or opportunities towards expand a outlooks, ‘KING855’ continues prepared regarding outdo a hopes various motion concerning a way. Uma dúvida comum que aparece cada vez mais entre os jogadores é relacionada a qual seria o melhor horário para jogar fortune tiger. Uma dúvida comum que aparece cada vez mais entre os jogadores é relacionada a qual seria o melhor horário para jogar fortune tiger. Sério. Ainda tá aqui por quê? Sobe essa página, escolhe um slot brabo e vai viver sua lenda pessoal em giros insanos. O Demo Slots Fun é o lugar onde heróis nascem girando!
https://btattoos.in/index.php/2025/06/03/1win-mines-demo-jogabilidade-e-beneficios-para-jogadores-brasileiros/
Antigamente, tinha todo um mito que falava sobre horários pagantes no Fortune Tiger. No entanto, como o jogo é totalmente aleatório, isso não é verdade. Agora pessoal, caso você tenha interesse em sempre estar atualizado nos horários que realmente estão pagando, acesse o site abaixo e tenha acesso ao FORTUNE TIGER CARTAS 10X, sempre os horários se atualizam..HORÁRIOS SEMPRE ATUALIZADOS DO FORTUNE TIGER! Uma dúvida comum que aparece cada vez mais entre os jogadores é relacionada a qual seria o melhor horário para jogar fortune tiger. No entanto, antes de se cadastrar em qualquer plataforma, é preciso escolher uma operadora confiável. Abaixo, listamos os melhores sites e as ofertas promocionais para quem quer jogar o Jogo Fortune Tiger, ou Jogo do Tigrinho e apostar. Separamos abaixo as cinco principais opções de casas para jogar:
Si eres de los que prefiere este momento del juego en el que la adrenalina corre por tus venas, entonces este juego sacará tu mejor hincha. Puedes buscar tácticas específicas para ganar en Penalty Shoot Out Street en línea o seleccionarlas tú mismo según tu estilo de juego. Hoy ya existen varios esquemas de trabajo listos para principiantes. Ante todo, es necesario entender que los juegos de azar siempre provocan un caleidoscopio de emociones. La alegría de la victoria es reemplazada por la decepción en la derrota. Para controlar tu reacción, debes prepararte de antemano. Es importante darse cuenta de que la cantidad en el saldo teóricamente puede perderse. Es mejor considerar las apuestas en Penalty Shoot Out Street como entretenimiento, con una pequeña posibilidad de aumentar el bankroll.
https://greenhillsaustralia.com/2025/06/03/resena-de-balloon-game-diversion-en-el-casino-online-para-jugadores-de-chile/
Blvd. Miguel de Cervantes Saavedra 161, Pisos 14 y 15, Granada, Miguel Hidalgo, 11520 Ciudad de México, CDMX, México Este juego Flash actualmente no se puede jugar en tu navegador, ¡pero estamos trabajando para solucionarlo! Vuelve regularmente para ver si está listo para jugar. This Wednesday sees the #PlayOffLaLiga get underway, with Gimnastic, Girona FC, Cordoba CF and At.Osasuna set to fight it out to claim their place in the Liga BBVA. Mantente conectado ¡Un clic para instalar archivos XAPK APK en Android! Como pateador, haga clic y deslice el balón con el mouse para realizar un tiro. ¡Ten cuidado, si deslizas demasiado lejos podrías perderte! Click Play to see the videoguide for Penalty Shooters Great score game for football fans Una buena opción para los principiantes será pasar a la versión demo de Penalty Shoot Out Street. La máquina se ofrece en modo gratuito, lo que permitirá probar el juego con créditos virtuales. A los jugadores se les dan 5000 fichas, con las que es fácil jugar sin restricciones. La ventaja es que podrás probar cualquier estrategia sin riesgo. Y luego, estas tácticas se transfieren a las rondas ya con dinero real.
The BharatPe app now offers a seamless and user-friendly way for consumers to make digital payments with ease. Colour trading apps like Tashan Win use an enjoyable and interesting method to make money online. By logging right into the application everyday and benefiting from its features, you can begin making money quickly and effectively. Whether you want colour trading, video games, or various other lucrative possibilities, Tashan Win supplies an interesting platform with the possibility for daily earnings. By adhering to the pointers discussed above and continually using the application, you can optimize your chances of success and appreciate the incentives that include mastering the colour trading app. Why wait? Log in to Tashan Win today and begin gaining online. Mutual fund investments are subject to market risks, read all scheme related documents carefully before investing. Dhan is not a distributor or agent of any mutual fund. Mutual Funds are not exchange-traded products. Any related disputes will not have access to the Exchange-investor redressal forum or arbitration mechanism. For other disclaimers please refer dhan.co advertisement-disclaimer
http://lienket.vn/5npfr
A total of 14 types of games are given in Game Free App APK. We have shown the names of all those games through the table in the article below. You read it and choose the game of your choice, the game you know about which can help you easily. You can play it and earn money.Every person in this world has a favorite game, some want to play cricket, some want to play football, some want to play hockey. Similarly, among all the games available in this app, our favorite game is Dragon vs Tiger. Choose which game is yours and play it.In Dragon vs Tiger, the decision is taken in a very short time and who wins and who loses is decided immediately, hence it is my personal game and even very less educated peo Friends, as soon as you do this process, you can get unlimited bonus from these slot apps and by playing games with the bonus money and making 100, you can transfer it to your bank account that too without any payment. deposited
Ich paar tausen plus machen das emfehle ich es jedem weiter lan Alles begann im Jahr 1983 und wurde sofort ein Hit. Wer würde nicht gerne zusehen, wie die Chips umherspringen, um eine Chance auf süße Preise zu haben? Nun, die Popularität von Plinko blieb nicht im Fernsehen hängen. Es stellt sich heraus, dass auch Online-Casinos und mobile Apps das Spiel lieben! Jetzt können Sie das klassische Plinko-Spielerlebnis von überall aus spielen, mit einigen modernen Vorteilen. Denken Sie an schicke Grafiken auf dem Brett, anpassbare Funktionen und sogar die Möglichkeit, in einigen Online-Casinos mit Kryptowährung zu spielen. Es ist der gleiche Spaß wie der Plinko-Spaß, den Sie kennen und lieben, aber mit einem digitalen Touch! Wir warnen dich eindringlich davor, dir Plinko Apps herunterzuladen, auch wenn die Anbieter damit werben Plinko seriös und mit enormen Gewinn spielen zu können. All diese Fake Apps haben nur das Ziel, deine Daten abzugreifen und zu Gewinnauszahlungen kommt es auch nicht.
https://www.fundable.com/jacqueline-cox
Das Spiel wird mit einem Kartendeck gespielt, können Sie Ihre Gewinnchancen erhöhen und mehr Geld gewinnen. Ein Willkommensbonus ist ein Angebot, und es gibt keine versteckten Bedingungen. Die beliebteste Variante ist Texas Holdem, ob Sie ein Android. NetEnt und Playtech, ein iOS. Plinko ist ein spannendes und einfaches Glücksspiel, das sowohl für Anfänger als auch für erfahrene Spieler attraktiv ist. Es bietet die perfekte Kombination aus Zufall und Strategie, wodurch jeder Spielmoment einzigartig wird. Wenn Sie in der Schweiz echtes Geld setzen möchten, folgen Sie den nachstehenden Schritten, um das Beste aus Ihrer Spielerfahrung herauszuholen. Erfolgreiches Spielen bei Plinko erfordert mehr als nur Glück. Ein gut durchdachter Einsatzplan ist entscheidend. Spieler sollten mit kleinen Einsätzen beginnen und diese schrittweise erhöhen, sobald sie ein besseres Verständnis für das Spiel entwickeln. Außerdem ist es ratsam, das Spiel in der Demoversion zu testen, bevor man echtes Geld einsetzt. Dies hilft, ein Gefühl für das Spiel zu bekommen und potenzielle Strategien auszuprobieren, ohne finanzielles Risiko.
Het is zover: de Oranje Jackpot van Pragmatic Play heeft de miljoen euro aangetikt! Deze jackpotfunctie werd in 2024 geïntroduceerd op gokkasten die enkel voor Nederlandse spelers beschikbaar zijn. Je kunt typisch Hollandse gokkasten spelen om kans te maken op de Giga jackpot, denk aan Sweet Bonanza Holland, Ik Wil Kaas en Kroonjuwelen. Gokkasten overzicht » Sweet Bonanza Sweet bonanza automatische spin en verlieslimiet Welk spel je ook speelt, win je de jackpot. Sweet Bonanza kent een tuimelfeature: winnende symbolen verdwijnen en maken plaats voor nieuwe symbolen. Zo gebeurt het regelmatig dat er binnen één spin meerdere keren winnende combinaties verschijnen. Er is geen limiet! Het spel is ontstaan in Frankrijk en heeft zich in de loop der jaren ontwikkeld tot een spannend en opwindend kansspel, niet alleen degenen die net hebben aangemeld bij dit casino. Gegroepeerd in verschillende categorieën, maar de bonus features zijn geweldig. Een avond vol entertainment bij het casino.
https://pitchwall.co/user/paracycpyou1983
Pragmatic Play heeft een breed scala aan spellen ontwikkeld, waaronder slots, live casinospellen en bingo. Enkele van hun populaire slots zijn Wolf Gold, Sweet Bonanza en The Dog House. Daarnaast bieden ze ook live casinospellen aan zoals blackjack en roulette. Bet365 is een gevestigde naam in de online gokwereld en heeft ook in Nederland een sterke positie. Het sportsbook is van topkwaliteit en biedt flexibele quoteringen en een breed aanbod aan sportweddenschappen. Het casinoproduct is echter minder indrukwekkend, met een beperkt en niet altijd aantrekkelijk spelaanbod. De klantenservice laat ruimte voor verbetering, met lange wachttijden en een gebrek aan lokale expertise. Betrouwbaarheid staat buiten kijf, maar de onduidelijke voorwaarden zijn een aandachtspunt. Al met al biedt bet365 een solide ervaring, vooral voor sportwedders. Daarom beoordelen wij bet365 met een 7.7 in de eindbeoordeling.
The Sweet Bonanza 1000 slot is a revamp of Sweet Bonanza which both are developed by Pragmatic Play. Sweet Bonanza was one of their most famous games but I would recommend others like The Dog House, The Wild Gang, and Twilight Princess. Sweet Bonanza Sweet Bonanza 1000 packs an extra feature buy option as well, which might be all the sweetener certain fans of the first need to get on board with the remake. This is a bigger game, fair enough, but in some ways, not so much bigger, theoretically speaking. Still, add everything up, and Sweet Bonanza 1000 ticks all the boxes required of a 1000 slot, offering all the things the original did, and more. The Sweet Bonanza 1000 slot is a revamp of Sweet Bonanza which both are developed by Pragmatic Play. Sweet Bonanza was one of their most famous games but I would recommend others like The Dog House, The Wild Gang, and Twilight Princess.
https://opendatabozp.cz/user/darseattmostper1979
If you’re looking for a casual game to fill the hours, Teen Patti Dhamal can be a great source of entertainment. This free online card game is based on Teen Patti, the well-loved Indian variation of poker. The game requires three or more participants and typically uses a standard 52-card deck. A free app for Android, by teenpatti cardgame. Yes, Teen Patti Master is free to download and play. However, you can buy extra chips and in-game items through in-app purchases. In 2023, Teen Patti Gold was updated with new game modes and unlimited rewards. You can now play with your friends or join tournaments with players from around the world. Teen Patti Sweet is an engaging online game that provides a new outlet for fans of the classic card game to enjoy their favorite pastime both at home and on the go. It allows players to compete with other participants worldwide for the chance to win the coveted pot of prize money. A player must have the highest three-card poker hand to win the game.